“I’m All Shook Up” The Vestibular System, Vertigo and the Role of Physical Therapy
By Jessica Lowy PT,DPT,CMTPT,SSOL Advanced Schroth Clinician, McKenzie A-D
Michal (Micky) Porath PT,MPT, SSOL Advanced Schroth Clinician, McKenzie A-D
Imbalance due to vertigo or dizziness is a diagnosis that we frequently treat in the clinic. Common complaints include “I get dizzy when I roll over in bed”, or “I get dizzy when I pick up something from the floor”. Sometimes these instances of vertigo or dizziness result in falls. Maintaining balance is the result of a complex integration of various sensory systems within the body, and the vestibular system plays a crucial role in this. The vestibular system, situated within the inner ear, is responsible for providing our brain with information about spatial orientation, equilibrium, and motion. When this system is compromised, individuals may experience dizziness, vertigo, and an increased risk of falls. Physical therapy offers a multifaceted approach, to help restore balance and conquer vestibular challenges.
Understanding the Vestibular System:
The vestibular system is comprised of the otolith organs and the semicircular canals, which work together to transmit signals to the brain about head position, movement, and gravitational forces. Disruptions in this system can lead to a myriad of vestibular disorders.
Common Vestibular Disorders:
Benign Paroxysmal Positional Vertigo (BPPV): This is characterized by brief episodes of dizziness triggered by specific head movements. Physical therapists often use repositioning maneuvers to guide displaced inner ear crystals back to their proper place, alleviating symptoms.
Meniere’s Disease: This chronic condition involves an abnormal buildup of fluid in the inner ear, leading to vertigo, tinnitus, and hearing loss. Physical therapy focuses on balance exercises and lifestyle modifications to manage symptoms.
Vestibular Neuritis and Labyrinthitis: Inflammation of the vestibular nerve or inner ear can cause severe vertigo. Physical therapy helps patients adapt to the changes in their balance and improve overall stability.
The Role of Physical Therapy in Vestibular Rehabilitation:
Physical therapists employ a targeted approach to rehabilitate the vestibular system and enhance overall balance. Here are some key components of vestibular rehabilitation:
Assessment and Diagnosis: A thorough evaluation of the patient’s medical history, symptoms, and physical examination is crucial for an accurate diagnosis. This may involve specific tests, such as the Dix Hallpike Maneuver, to assess inner ear dysfunction, eye movements, head and body coordination, and positional changes.
Customized Exercise Programs: Based on the individual’s needs and specific vestibular disorder, physical therapists design personalized exercise regimens. These exercises often include gaze stabilization, habituation exercises, and balance training to improve coordination and stability.
The following exercise is an example of a VOR (vestibular ocular reflex) exercise used for gaze stabilization.
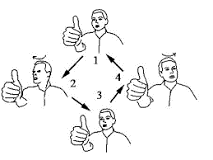
- Eye movements — at first slow, then quick. up and down. from side to side. focusing on finger moving from 3 feet (1 metre) to 1 foot (30 centimetres) away from face.
- Head movements at first slow, then quick, later with eyes closed. bending forward and backward. turning from side to side.
The Epley maneuver is used for treating BPPV (this is dependent on the side of the BPPV)
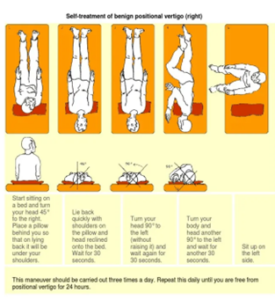
Adaptation and Compensation: Patients are guided through activities that challenge the vestibular system, promoting adaptation and compensation for any deficits. This helps the brain adjust to the altered sensory input and enhances overall function.
Patient Education: Understanding the vestibular system and how specific exercises contribute to rehabilitation is empowering for patients. Education on lifestyle modifications, fall prevention strategies, and coping mechanisms is an integral part of the therapeutic process.
Progress Monitoring: Vestibular rehabilitation is an ongoing process, and physical therapists continually assess progress and make adjustments to the treatment plan as needed. Regular monitoring ensures that patients are moving towards their goals and regaining control over their balance.
Physical therapy stands as a cornerstone in the management of vestibular disorders, offering a holistic and patient-centered approach to rehabilitation. By addressing the root causes of imbalance and dizziness, physical therapists empower individuals to regain control over their lives and navigate the world with confidence. As our understanding of the vestibular system continues to deepen, the role of physical therapy in revitalizing balance remains indispensable.
At Prime Orthopedic Rehabilitation, we have both male and female therapists. Our therapists all hold advanced certifications to help with your specific needs, including OCS certification, Orthopedic Certified Specialist. We offer general outpatient physical and occupational therapy, both In-Office and In-Home, but we also offer specific approaches such as McKenzie rehab for neck and back issues, Schroth approach for scoliosis, Vestibular rehab for dizziness, balance issues and vertigo, Sports rehab for sports injuries such as those from basketball or hockey, as well as therapists certified in dry needling, cupping, instrument assisted soft tissue mobilization (IASTM) and other approaches. Prime also has seventy 5-star google reviews and offers more one on one time than most other offices. Call us today to ask how we can help you 201-503-7173.
Jessica Lowy, DPT, CMTPT, DN, Mckenzie A-D, Advanced Schroth Clinician and Michal Porath, MPT, Mckenzie A-D, Advanced Schroth Clinician are owners of Prime Orthopedic Rehabilitation in Tenafly, NJ. They treat general orthopedic and post surgical patients, in addition to children and adults with scoliosis. Call (201) 503-7173 for an appointment.
Disclaimer
The medical/health information is provided for general informational and educational purposes only and is not a substitute for professional advice. Accordingly, before taking any actions based upon such information, we encourage you to consult with the appropriate professionals. The use or reliance of any information contained on this site is solely at your own risk. All information on this site is provided in good faith, however we make no representation or warranty of any kind, express or implied, regarding the accuracy, adequacy, validity, reliability, availability, or completeness of any information on this site.
